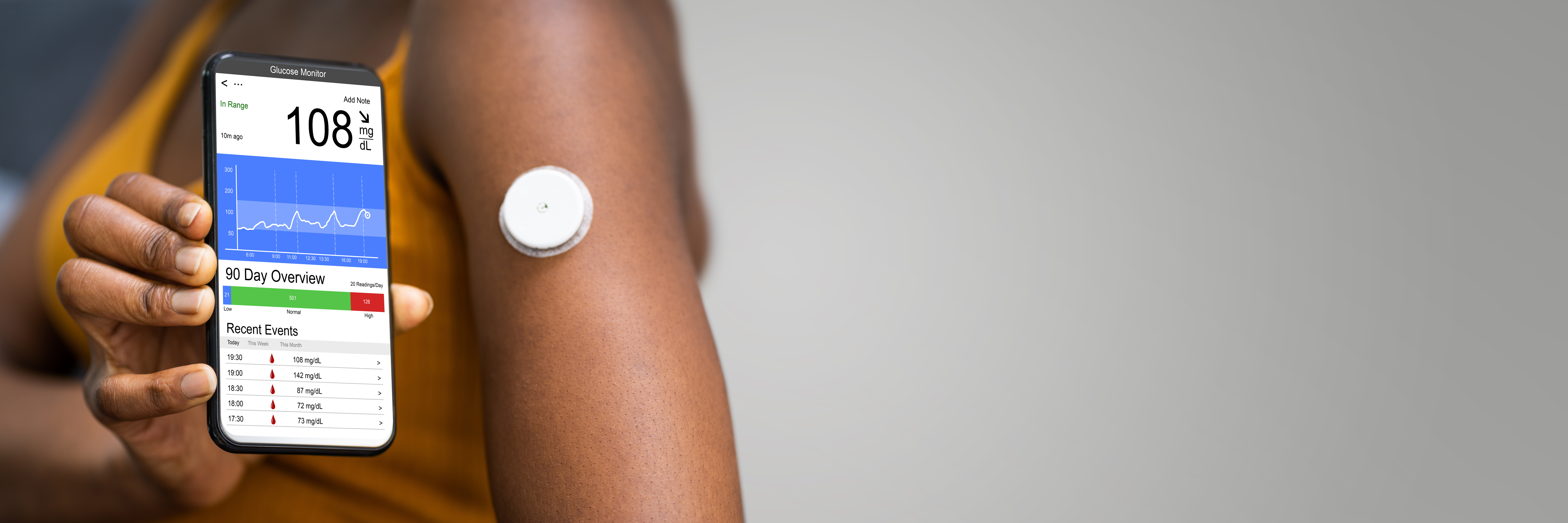
A ‘culturally appropriate’ approach to healthcare for Indigenous Australians using telehealth was the theme of a research study in 2018. [i]
The paper described ‘culturally appropriate’ healthcare as care that recognises the social, political and economic factors that affect health and access to healthcare.
In addition, considerations of dignity, privacy, safety, and the reduction of discrimination were considered within the term ‘culturally appropriate’.
RPM defined as capturing patient measurements using electronic devices is generally found to be most effective when coupled with Telehealth (The ability to interact visually with the patient via teleconferencing).
In this study, nine Aboriginal community controlled health services (ACCHS) staff members were interviewed about the possibility of developing culturally appropriate services more sensitive to the needs of this particular population.
ACCHS provides holistic and culturally appropriate healthcare to local Indigenous communities.
Through identifying, analysing and interpreting patterns one central theme and three sub-themes were identified.
The central theme explains how the supportive and safe environment of an ACCHS centre enables specialist telehealth consultations to take place instead of in a mainstream hospital.
 The three sub-themes described:
The three sub-themes described:
- How telehealth improved affordability and convenience and brought a reduction in the stress of healthcare.
- The importance of the presence of an Indigenous health worker to facilitate culturally appropriate healthcare.
- How telehealth supported a holistic view of health.
The study found that the use of telehealth may enhance culturally appropriate healthcare because it allows care to be provided in the supportive environment of an ACCHS.
Additionally, it allows the community member to have the advocacy and assistance of an Indigenous health worker and it reduces the burden of travel and dislocation from community and family.
But let’s expand the usefulness of telehealth to facilitate the broader implications of remote patient monitoring.
Remote patient monitoring refers to using specific technologies to facilitate interaction between clinicians at a Practice and patients at home.
According to a new report, investigator Professor Len Gray and researchers at The University of Queensland’s Centre for Health Services Research & Centre for Online Health said successful RPM programs are not usually just surveillance of data. [ii]
A combination of monitoring biometric measurements and telephone coaching, video consultations with nurses, care coordinator check-ins, and patient feedback is provided.
In many systematic reviews, researchers found that patients benefit from RPM over standard care. RPM reduces mortality, especially in relation to heart failure. [iii]
The health of Aboriginal and Torres Strait Islander people is at risk from cardiovascular disease and Chronic obstructive pulmonary disease (COPD) is a significant cause of hospitalisation and the leading cause of death among Indigenous people. [iv]
RPM interventions can improve clinical outcomes for patients while reducing the burden on health services by significantly reducing re-admissions. In a review of published studies on RPM, over 75% reported the intervention was effective. [v]
The statistics show that patients who have home remote monitoring devices saw a decrease of 44% in emergency admissions, 59% decrease in cost of care and connected health is 40% cheaper than face-to-face. [vi] [vii]
Many different RPM programs funded by governments or private health insurance payers exist internationally, yet Australia is falling behind.
It is our vision at RPM-H to empower patients and clinician staff through interconnected, preventative, and proactive care whilst continuing to live independently and healthily in the most appropriate location.
For further information about leading RPM software, visit our website www.rpm-h.com.au or contact us below.
Contact Form
[i] https://journals.sagepub.com/doi/epub/10.1177/1357633X18795764
[ii] https://healthsystemsustainability.com.au/international-remote-patient-monitoring-programs-and-health-system-sustainability/
[iii] https://pubmed.ncbi.nlm.nih.gov/19850208/
[iv] https://healthinfonet.ecu.edu.au/learn/health-topics/cardiovascular-health/
[v] https://pubmed.ncbi.nlm.nih.gov/31314689/
[vi]https://static1.squarespace.com/static/5b67adf2af2096c5aae0d566/t/5fda9fa23c596733c68781ec/16081632
[vii] https://digitalhealth.org.au/slides/hic17/tue/LisaCapamagian.pdf